Technology to Bring high quality neuro-rehabilitation in every home guided by Active Assistance
The Motus Hand and Foot are FDA Class 1 at-home stroke rehab robots in the world with active assistance. Scientific studies have shown The Motus Hand and Foot induce equivalent functional improvements to those observed with standard clinical care. Motus technology uses high-dose repetitive task practice to help stroke survivors improve hand and foot function.
Using theMotus Hand for recovery
“leveraging technology and active assistance for access to stroke rehab at home”
Safe and Effective: Dozens of Scientific Publications and a decade of clinical research
Designed to work at home
Built for Independent Use
The Motus Hand and Foot can be used without needing help from a clinician or caregiver. The robot and the monitor can be operated by the stroke survivor so you can do your rehab when it is most convenient for you.
Patented Assistive Technology
The device is connected to a pneumatic actuator — an air pump — that assists the user when necessary.
Our stroke rehabilitation technology tracks movement activity during therapy and provides assistance when the user is struggling to finish a complete movement.
Personalized Rehab
The monitor that connects to the device displays games which provide the user with an interactive way to do their therapy.
The Motus system constantly tracks and monitors user recovery so that it can adjust the level of assistance and resistance based on individual user needs.
Biofeedback
The Motus Hand & Foot sensors detect when you’re making correct movements. A signal is provided when you complete a correct movement. Over time a user is able to recognize these signals and be able to recreate the movement.
Get more repetitions with games designed to keep you engaged for hours.




Consistent repetitive use of impaired limbs
Repetition is the single best way to continue improving movement after stroke. Motus games keep you engaged for hours so you can pack in a high number of repetitions.
Relearning simple motor activities
Stroke recovery can be a long process of relearning how to walk or eat independently. Motus games help you get there faster by increasing your hours of therapy.
Reduced depression and stronger motivation
Boring home exercises demotivate survivors which can lead to depression. Motus games can keep you engaged for hours by stimulating your brain leading to reduced depressive symptoms and better motivation.
Reporting
Track your progress in real time
Total Hours
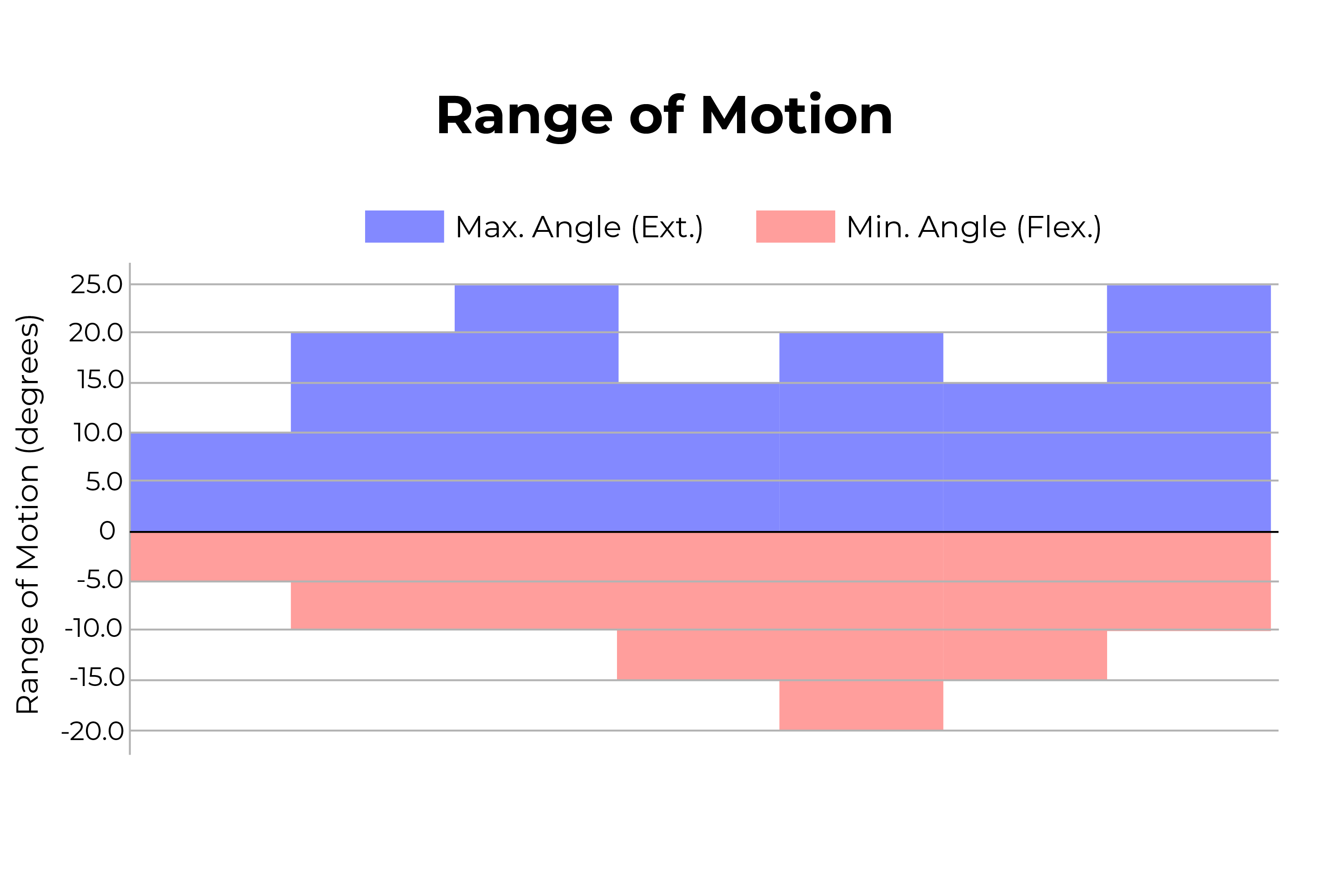
Range of Motion
Strength
Endurance
“One thing I love to do is after I do a session with the Hand I like to generate the report so I can see how many repetitions I’ve done and that’s been very helpful.”